Assalamualaikum.
Just to share the pregnancy and birth story of our miracle baby :-)
Hopefully it inspires other families to consider more on gentle birthing, InshaAllah.
First Trimester:
Got to know I was pregnant just a 4 weeks. Could feel some changes such as light headedness and increase olfactory sensations. Did a UPT and it was confirmed :-) Shared the news with Hubby, family and some friends.
It was indeed a miracle since just few weeks before that, I got really interested to know more on gentle birthing, bought the AMANI Birth book & so inspired by it and some of the gentle birth stories I read. As I was wishing to experience a gentle birth someday, Alhamdulillah, Allah blessed us with this new pregnancy!
Surveyed for a healthcare provider and the options we had for antenatal care and birthing. My hubby was new to gentle birthing concept but he just kindly agreed to my wishes.. Alhamdulillah, heard so much about Dr.Idora from Pantai KL and decided to make an appointment to meet her at 7 weeks pregnancy. She seemed to be supportive of my ideas of birthing Alhamdulillah, so we decided to continue with her throughout the pregnancy.
My only drawback at first trimester was having GERD annd terrible vomitting until I lost 5kg during the first trimester. At first, I tried my best not to take any medications and tried all sorts of natural remedies like ginger, honey etc. None seemed to work, and with worry that I might not provide enough nutrients for my baby, I resorted to taking PPI for 2 weeks. Alhamdulillah, at 14 weeks pregnancy, vomitting resolved and appetite caught up :-)
2nd Trimester
Blissfully uneventful. Found out we were expecting a boy at 15 weeks POA. Felt fetal kick at 16 weeks POA while performing terawikh on 1st Ramadhan during 1st rakaat Terawikh. Alhamdulillah managed to fast the whole month of Ramadhan.
Did Antenatal Exercises like Tailor Sitting, Squats, Walking on Treadmill & Belly dancing.
Alhamdulillah felt perfectly healthy during my 2nd trimester. Happy that I got to resume with daily chores as usual.
3rd Trimester
Pressure symptoms like pelvic pressure, frequent urination and sciatica catching up. Many sleepless nights & indeed exhausted. Slowed down on exercise, just did normal household stuff like cooking, light walking here & there and concentrated more on Kegel exercise. Getting excited & nervous at the same time :-)
THE BLISSFUL BIRTH STORY
Sunday, 30 November
4 a.m: Woke up with painful surge. Timed surges around 1 in 10.
6 a.m: Waited for Subuh, showered and prayed. Applied clary sage essential oil on my ankles to help increase surges. Went to sleep soon.
10 a.m: Woke up with surges again. Told hubby about it. We called labour room to book a waterbirth suite for us.
4 p.m: Arrived at labour room. CTG showed contractions 1 in 6. Upon VE, I was told cervix was still posterior & only 1 cm dilated. Adviced to go home & rest, let nature takes it course.
Feeling a bit dissapointed, we went hime tht day.
Next 2 days was just the same. I was restless & exhausted with on & off contractions.
On Tuesday night, 2nd December, Hubby let me rest alone in our room while he took tge kids to another room to sleep. I on the diffuser & put some Balance Essential Oil in it. Again applied clary sage oil on my ankles. Alhamdulillah, I got such wonderful sleep that nightt.
Wednesday, 3rd December 2014
1 p.m: Felt surges becoming stronger. Rested on bed after Zuhur prayers.
5 p.m: Woke up with painful surges again. Told hubby & we decided to go to labour room after Magrib prayers.
9 p.m: Contractions showed 1 in 3 at labour room. Upon VE, cervix still only 1cm. I was upset but Hubby was convinced that I was in true labour this time around. We stayed on in labour room that night.
Hubby on the diffuser with Balance essential oil.
Time to time he fed me with dates & also let me drink
"Air Bunga Fatimah". Both are supposed to provide energy & help with muscle contractions.
12 a.m: Surges getting stronger. I was so restless, walking around the room & squatting with each surge. I felt squatting helps to relief pain & also help open pelvic outlet to descend baby. I called the midwive for VE. Still no progress..definitely was upset but hubby told me to stay strong & reminded me, every surge is bringing us closer to the baby..
Hubby put on the Ocean Serenade music to keep me calm while he dozed off a while. I worked on tolerating the contractions, reminding myself not to fight the pain but to work with it as it serves as a purpose (to help me bring out the baby). I tried relaxing all the muscles including my jaws while the contractions came so that all energy can be focused on the uterus doing its job. This went on until 6 a.m.
6 a.m: Cleared my bladder & requested for VE. Had some bloody show. Upon VE, dilated 3cm. Hubby informed the nurses that I am a fast progresser once dilated. They got the water tub ready for me. He also applied Helichrysium Essential Oil on my back to prevent hemorrhage.
8.30 a.m: Was in so much pain, started losing control. Upon VE was 5 cm dilated.
Started behaving differently & was in so much pain. Thank God hubby was with me all the way, holding my hand, rubbing my back & praying for me.
9 a.m: Dr arrived. VE 7cm. Was told that I could get in the water tub.
They nurses helped me into the tub.
Subhanallah, the warm water was such a pain relief!!
They on the Ocean Serenade music again to comfort me.
The nurses kept on pouring warm water and comforting me.
Dr Idora was so gentle with her words. I remember her saying " Just go with the urge". & " Keep breathing well "..
9.15 a.m: Felt urge to bear down. I was in a sitting reclining position.
wanted to squat but had no more energy to do so.
With each surge, I breathe my baby out into the world.
Hubby was there stroking my head and saying kind words. After few pushes, my baby's head was out along with his amniotic sac. It broke when he was halfway out.
9.20 a.m: Baby was out & on my chest. Muhammad Saiful Islam was born at 3.14kg.
We came out of the tub & Dr. Idora started stitching me soon (I had just 2 stitches for some superficial tear).
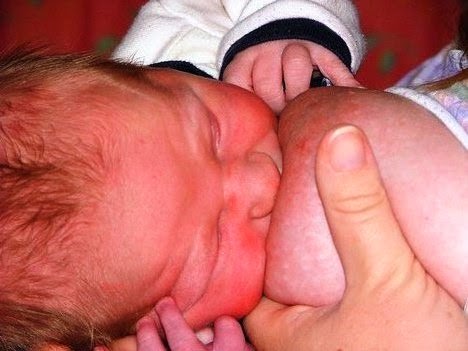
while stitching was going on, my baby latched like a champion, Alhamdulillah. He did the breast crawl thing & found his way to latch!
Soon the cord dried out (we had about 10 minutes of delayed cord clamping) and my hubby was given the honour to cut the cord. Few seconds later, felt the urge to push out the placenta & it was out naturally.
We then had 2 hours of skin to skin time.
Alhamdulillah, felt so empowered and refreshed by this experience. Hubby seemed amazed too & mentioned he was proud that I did it without anaesthesia! To me, he was my pain relief..nothing can beat a loving support during labour!
p/s: Couldnt have done it without my hubby! Special credits to all who supported & encouraged me towards gentle birthing. Love u Mummies!
Friday, 5 December 2014
Wednesday, 1 October 2014
Diet 'can flavour mother's milk'
Adapted From: http://news.bbc.co.uk/2/hi/health/7521750.stm
Thursday, 19 June 2014
A Natural Protein in Breastmilk That Fights HIV
For decades, public health officials have puzzled over a surprising fact about HIV: Only about 10-20 percent of infants who are breastfed by infected mothers catch the virus. Tests show, though, that HIV is indeed present in breast milk, so these children are exposed to the virus multiple times daily for the first several months (or even years) of their lives.
Now, a group of scientists and doctors from Duke University has figured out why these babies don’t get infected. Human breast milk naturally contains a protein called Tenascin C that neutralizes HIV and, in most cases, prevents it from being passed from mother to child. Eventually, they say, the protein could potentially be valuable as an HIV-fighting tool for both infants and adults that are either HIV-positive or at risk of contracting the infection.
The research, published today in Proceedings of the National Academy of Sciences, was inspired by previous work by other researchers showing that, both in tissue cultures and live mice, breast milk from HIV-negative mothers was naturally endowed with HIV-fighting properties. Scientists suggested that a few different proteins in the milk could potentially be responsible, but no one knew which one.
As part of the study, the researchers divided breast milk into smaller fractions made up of specific proteins via a number of filters—separating the proteins by size, electrical charge and other characteristics—and tested which of these fractions, when added to a tissue culture, prevented the cells from being infected by HIV. Eventually, using mass spectrometry, they found that one particular protein was present in all the HIV-resistant fractions but in none of the others: Tenascin C.
“The protein works by binding to the HIV envelope, and one of the interesting things is that we were even able to narrow down exactly where on the envelope it binds,” says Sallie Permar, the study’s lead author. Her team found that the protein binds to a crucial region on the virus’ envelope that normally locks onto a receptor called CCR5 on the outside of human T cells,allowing it to fuse its membrane with the cell’s. With the region covered up by Tenascin C, HIV’s normal route of attack is blocked, and the virus’ effectiveness is greatly diminished.
Still, the researchers say that other natural elements in milk might play a role in fighting HIV as well. “It’s clearly not the whole story, because we do have samples that have low amounts of this protein but still have HIV-neutralizing activity,” Permar says. ”So it may be acting in concert with other antiviral and antimicrobial factors in the milk.”
Whatever those other factors are, though, the finding vindicates recent changes to UN guidelines that recommend even HIV-positive mothers in resource-poor countries should breastfeed, if they’re taking anti-retroviral drugs to combat their own infection. That’s because—as statistics bear out—the immense nutritional and immune system-boosting benefits of breast milk outweigh the relatively small chance of transmitting HIV through breastfeeding. Tenascin C, it seems, is a big part of why that transmission rate is surprisingly low, and sufficient access to anti-retroviral drugs can help drive it even lower—as low as 2 percent.
The next steps, Permar says, are determining which area of Tenascin C is active in binding to HIV and whether it can effectively prevent transmission in a live animal, as opposed to a tissue culture. If it works, it could potentially be incorporated into an HIV drug with broader applications. Possible uses include giving it in a concentrated form to infants who can’t breastfeed or even administering it to those who do to increase their level or resistance. It’s even conceivable that it could someday be adapted to reduce the risk of HIV transmission in adults as well.
One immediate advantage, says Permar, is that “it’s like to be inherently safe, because it’s already a component for breast milk. It’s something babies eat everyday.” Other potential treatments, on the other hand, must be screened for toxicity.
Tenascin C’s presence in breast milk, though, prompts a deeper question: Why would milk naturally include a protein that battles HIV, a virus that evolved extremely recently in our evolutionary history, sometime in the early 20th century?
“I don’t think it’s in breast milk to combat HIV specifically, but there have been other, related infections that have passed through breastfeeding,” Permar says. “Our work has shown that Tenascin C’s activity isn’t specific to HIV, so we think it’s more of a broad-spectrum anti-microbial protein.”
In other words, Tenascin C is effective at combating a large variety of infections (perhaps related to its role in adults, where it holds various types of tissue together, necessitating receptors that can bind to a wide array of different cells). The fact that it happens to bind at just the right spot on HIV’s outer envelope so that it combats the virus’ transmission, as Permar puts it, is “a gift from evolution.”
Original article from: http://www.smithsonianmag.com/science-nature/discovered-a-natural-protein-in-breast-milk-that-fights-hiv-3189537/?no-ist
Monday, 9 June 2014
Mother's Rights to Work, Worker's Rights to Motherhood
Assalamualaikum/Greetings!
On the 5th of June 2014, I had the chance to attend the Lactation Management Workshop at the 23rd Congress of Obstetrics & Gynaecology Society of Malaysia.
The Theme was: Mother's Rights to Work, Worker's Rights to Motherhood
I sincerely would love to share this information with women out there for you to know your rights as a breastfeeding mother.
The information which I am going to disclose here was presented at the congress and is adapted from the following file. Do read it if you have the time to do so :-)
http://www.waba.org.my/whatwedo/womenandwork/pdf/02.pdf
So what are the ILO Recommendations for future Maternity Protection? (R191)
Below are some things Medical Proffessionals can help to assist in helping a working mother achieve successful breastfeeding:
On the 5th of June 2014, I had the chance to attend the Lactation Management Workshop at the 23rd Congress of Obstetrics & Gynaecology Society of Malaysia.
The Theme was: Mother's Rights to Work, Worker's Rights to Motherhood
I sincerely would love to share this information with women out there for you to know your rights as a breastfeeding mother.
The information which I am going to disclose here was presented at the congress and is adapted from the following file. Do read it if you have the time to do so :-)
http://www.waba.org.my/whatwedo/womenandwork/pdf/02.pdf
Maternity protection at the workplace is a legal and social recognition of the contribution that women make by having babies. The International Labour Organization (ILO) first recognised the importance of maternity protection in 1919 in its third convention (C3). In 1952, a second ILO maternity protection convention was adopted (C103), and in 2000 a third.
During the 20th Century, most countries of the world have enacted maternity protection legislation at national level.
Seven Key Elements of Maternity Protection are:
1. Scope
-Covers all employed women including those in atypical forms of dependent work (meaning those in part time, temporary work who have an employer).
2. Leave
-Length of leave increase from 12 weeks to 14 weeks. (compulsory 6 weeks postnatal leave).
3. Benefits
-Cash benefits of no less than 2/3 of salary.
-Prenatal, childbirth and post-natal care and hospitalization
where necessary.
where necessary.
4. Health Protection
- protection for women and their babies from hazards in the workplace
5. Job Protection
- Job protection and non-discrimination: holding a woman’s job or a job at the same level to which she can return after leave; forbidding discrimination on the grounds of maternity
6. Breastfeeding Breaks
- A woman has the right to one or more daily paid breaks for breastfeeding or a daily reduction of working hours.
7. Breastfeeding Facilities
- a place where a worker can feed her baby or express her milk
The ultimate goal is to have these elements implemented as a minimum standard in national legislation on maternity protection.
Do correct me if I am wrong, but currently in Malaysia, maternity protections has not reached the level of "LEGISLATION" yet. This is what we as Breastfeeding Advocates are currently aiming for and working towards it step by step.
Below are the comparisons of Maternity Leaves and practice of Breastfeeding Breaks in various countries:
So what are the ILO Recommendations for future Maternity Protection? (R191)
Below are some things Medical Proffessionals can help to assist in helping a working mother achieve successful breastfeeding:
Sunday, 8 June 2014
My 2nd Pregnancy & Birth Story
Assalamualaikum :-)
I am indeed sorry that I took such a long time to write up this 2nd birth story.
FINDING OUT ABOUT THE PREGNANCY:
I found out I was pregnant with my 2nd one at about 5 weeks of gestation. The line on the pregnancy test I took was really faded, so I took another test 1 hour later ( I was working in a clinic at that moment, so it was convenient for me to grab another test right away :-) ) The other test was also faded, but both tests did darken with time.
As a working doctor, with ultrasound at the clinic at that time, I decided to do an ultrasound right away on myself (too excited!). And indeed I saw a gestational sac! Was so excited, over the moon, MashaAllah!
We really wanted a sibling for my eldest daughter.
I went for my first antenatal check-up with OBGYN. Everything seem normal at that time except that I started having quite sever nausea and vomiting.
THREATENED MISCARRIAGE:
At about 7th week of gestation, while I was bathing my eldest daughter, suddenly I felt a sharp lower abdominal pain, and a gush of blood came..and the amount was so scary! It was literally a pool of fresh blood! I called for my mother in law and hubby who came rushing to help me lie down on the bed.
I was a bit panicked at that moment of time even though I experienced similar bleeding problem with my first pregnancy. However, this time around, the bleeding came gushing with fresh blood as compared to menses-like bleeding the first time around. We went to the hospital that night and at the ER they gave me a progesterone jab along with some progesterone tablets to start on. Ultrasound showed subchorionic bleed and there was fetal heartbeat (so I was relieved!).
A week went by, and the bleeding subsided Alhamdulillah!
APPENDICITIS IMPENDING RUPTURE:
As for my nausea and vomiting, it started at about 6 weeks gestation but became worse at about 10 weeks gestation. I was wondering why it became worse when it was supposed to subside with time..
It came to a point when I could not even take liquids, I would throw everything up..and I had this aching pain at my right hypochondrial area for a few days..went to the OBGYN but could not find anything on her ultrasound..she suggested I make an appointment with the radiological department for further detailed ultrasound of the abdomen..
Next day, while I was at work, I developed fever with nausea, vomiting and chills. Went to the ER and they referred me to radiological department after taking my blood for blood tests. According to the radiologists, they saw my appendix was swollen with fluid around it and alerted the surgeons. I was scheduled for an emergency appendicectomy and was put on General Anaesthesia (because the appendix will most likely rupture if they do not remove it, and that could be fatal for me) . Only God knows how worried I was at that moment, a surgery under general anaestesia at 12 weeks gestation! But the benefits outweighed the risks and my husband and I surrendered to Allah Almighty to save me and the baby.
Alhamdulillah, surgery went well, I recovered quite fast and was able to eat and drink normally again! Ramadhan came along soon after that, and Alhamdulillah, I managed to fast for the whole month without missing a day :-)
PREGNANCY INDUCED HYPERTENSION & LEAKING LIQUOR:
I gave birth to Nur Nabeeha while she was just 36 weeks of gestation..which is 4 weeks earlier than my expected due date.
Just two weeks before giving birth, which is about 34 weeks of pregnancy, I found out that I had pregnancy-induced Hypertension..which was quite a surprise for me as my blood pressure had always been on the lowish side. I was negligent too I guess, was too confident that everything is fine and was busy with household stuff and work that I neglected my last follow up and went for check-up two weeks later..It was an irony too, because I was working in a clinic at that time, and the blood pressure machine was always just beside me all the time, but never did I bother to check on my blood pressure!!
So anyway, doctor told me to monitor my blood pressure 4 times daily and get plenty rest, and didn't start me on any medication yet.
Besides the hypertension, I also started to leak some liquor (that's the main reason I went for the check-up that day)..So again, I was told to monitor the leaking and given a follow-up the following week.
Interventions were taken that day too, like steroid injections for baby's lung maturity (just in case I deliver earlier that 36 weeks..) The doctor was hoping to buy some time before planning to induce my delivery until baby is 36 weeks and until more that 2kg..(at that moment of time, she was merely 1.8kg)..
So a week went by and I went for my follow up the following weeks..still leaking, and blood pressure fluctuating. So the OBGYN suggested to induce delivery on the 29th of December 2011 and although we were reluctant with the thought of induction, at that point of time, that was what we thought was the right thing to do in the best interest of the baby..
THE LABOUR :
The following morning after the check-up, I woke up for Fajr prayers, and realized that my waterbag has broken..It was about 6.45am..I woke hubby up and told him..
Then I packed up my hospital bag..and also packed up my elder's daughter bag (to send her to her grandma's).
I told hubby to get some rest as it's gonna be a long day :-)
Then he woke up at about 9.30a.m, saying he's worried that I would be in pain and couldn't sleep anymore. At that point of time, I had no pain yet, just discomfort from the water gushing out.
So we had roti canai for breakfast, and left house at about 11 a.m. We sent off my elder daughter and the maid to my MIL before going to the hospital.While on the way, I took sips of water which I soaked Bunga Kembang Fatimah with (it's suppose to help to accelerate labour).
We reached hospital at about 12 p.m and went straight to labour room. I felt my first contraction while we were in the car. At the labour room, the midwife checked and said that it was going to be a long way till delivery because cervix wasn't favourable at all..At about 1pm, my OBGYN came and did a V.E. She said I was already 2cm open..Alhamdulillah! However, she suggested that I was started on Pitocin to speed up the labour (with the reasons that I had been leaking liquor for some time and she did not want any infection to develop if the labour took "too long". She also was worried that a long labour might accentuate my hypertension). At that moment, I consented.
So she asked if i wanted epidural..I declined because I didn't like the idea of a needle poking nearby my spinal cord and also didn't want the side effects afterwards. I didn't take it for my first delivery, so I thought probably I might not need it this time as well..
At about 2p.m, I felt intense pain, and was already 3cm open. I requested for pethidine, and was given a shot. My BP shot up at that moment of time too so they gave me some anti-hypertensives and off the lights and told me to rest..
After that, I couldn't remember quite clearly anymore..All I knew was I keep waking up because of the intense pain..and at about 5pm, was told that I was 5cm open..and about 30 minutes later, I felt like pushing already..I told the nurse to check and to her surprise, I was already fully dilated and baby's head was ready to pop out..
So I started pushing, but to my despair, the nurse took a sanitary pad and blocked the opening, told me to stop pushing until the OBGYN comes. I was so angry at that point, I started shouting away. Luckily, the OBGYN arrived soon and only after 1 push, the baby was out! Alhamdulillah, I heard her cry and all the pain went away after that. To my delight, I was told that perineum was intact and no stitches were needed.
I was saddened that they did not allow me skin to skin time with my baby with the excuse that baby was small and had to be put to warmer. It really did hurt me but I was too weak to fight for it at that moment.
All I was thinking about was how glad I was to have delivered a healthy baby!
So overall, my active phase of labour this time was only about 5 hours, Alhamdulillah..compared to the 12 hours the previous time. I probably could give some credit to me making a habit to walk at least 15 minutes daily this time around :-) Hubby was there all the way beside me, giving me support and reminding me to be patient and salawat as much as I can..He was a gem at that moment, I cound't thank him enough..I held his hand all the way through the contraction pains..
Alhamdulillah for the fast and safe delivery :-)
As for my blood pressure, it went back to normotensive state about 2 weeks post-partum :-)
Even with the bad experiences during the labor this time around, I am thankful for a safe delivery and healthy baby, Alhamdulillah!
The past two birth experiences has encouraged me to look deeper into Gentle Birthing and hopefully I get a peaceful, calm gentle birth the next time around, InshaAllah!
I am indeed sorry that I took such a long time to write up this 2nd birth story.
FINDING OUT ABOUT THE PREGNANCY:
I found out I was pregnant with my 2nd one at about 5 weeks of gestation. The line on the pregnancy test I took was really faded, so I took another test 1 hour later ( I was working in a clinic at that moment, so it was convenient for me to grab another test right away :-) ) The other test was also faded, but both tests did darken with time.
As a working doctor, with ultrasound at the clinic at that time, I decided to do an ultrasound right away on myself (too excited!). And indeed I saw a gestational sac! Was so excited, over the moon, MashaAllah!
We really wanted a sibling for my eldest daughter.
I went for my first antenatal check-up with OBGYN. Everything seem normal at that time except that I started having quite sever nausea and vomiting.
THREATENED MISCARRIAGE:
At about 7th week of gestation, while I was bathing my eldest daughter, suddenly I felt a sharp lower abdominal pain, and a gush of blood came..and the amount was so scary! It was literally a pool of fresh blood! I called for my mother in law and hubby who came rushing to help me lie down on the bed.
I was a bit panicked at that moment of time even though I experienced similar bleeding problem with my first pregnancy. However, this time around, the bleeding came gushing with fresh blood as compared to menses-like bleeding the first time around. We went to the hospital that night and at the ER they gave me a progesterone jab along with some progesterone tablets to start on. Ultrasound showed subchorionic bleed and there was fetal heartbeat (so I was relieved!).
A week went by, and the bleeding subsided Alhamdulillah!
APPENDICITIS IMPENDING RUPTURE:
As for my nausea and vomiting, it started at about 6 weeks gestation but became worse at about 10 weeks gestation. I was wondering why it became worse when it was supposed to subside with time..
It came to a point when I could not even take liquids, I would throw everything up..and I had this aching pain at my right hypochondrial area for a few days..went to the OBGYN but could not find anything on her ultrasound..she suggested I make an appointment with the radiological department for further detailed ultrasound of the abdomen..
Next day, while I was at work, I developed fever with nausea, vomiting and chills. Went to the ER and they referred me to radiological department after taking my blood for blood tests. According to the radiologists, they saw my appendix was swollen with fluid around it and alerted the surgeons. I was scheduled for an emergency appendicectomy and was put on General Anaesthesia (because the appendix will most likely rupture if they do not remove it, and that could be fatal for me) . Only God knows how worried I was at that moment, a surgery under general anaestesia at 12 weeks gestation! But the benefits outweighed the risks and my husband and I surrendered to Allah Almighty to save me and the baby.
Alhamdulillah, surgery went well, I recovered quite fast and was able to eat and drink normally again! Ramadhan came along soon after that, and Alhamdulillah, I managed to fast for the whole month without missing a day :-)
PREGNANCY INDUCED HYPERTENSION & LEAKING LIQUOR:
I gave birth to Nur Nabeeha while she was just 36 weeks of gestation..which is 4 weeks earlier than my expected due date.
Just two weeks before giving birth, which is about 34 weeks of pregnancy, I found out that I had pregnancy-induced Hypertension..which was quite a surprise for me as my blood pressure had always been on the lowish side. I was negligent too I guess, was too confident that everything is fine and was busy with household stuff and work that I neglected my last follow up and went for check-up two weeks later..It was an irony too, because I was working in a clinic at that time, and the blood pressure machine was always just beside me all the time, but never did I bother to check on my blood pressure!!
So anyway, doctor told me to monitor my blood pressure 4 times daily and get plenty rest, and didn't start me on any medication yet.
Besides the hypertension, I also started to leak some liquor (that's the main reason I went for the check-up that day)..So again, I was told to monitor the leaking and given a follow-up the following week.
Interventions were taken that day too, like steroid injections for baby's lung maturity (just in case I deliver earlier that 36 weeks..) The doctor was hoping to buy some time before planning to induce my delivery until baby is 36 weeks and until more that 2kg..(at that moment of time, she was merely 1.8kg)..
So a week went by and I went for my follow up the following weeks..still leaking, and blood pressure fluctuating. So the OBGYN suggested to induce delivery on the 29th of December 2011 and although we were reluctant with the thought of induction, at that point of time, that was what we thought was the right thing to do in the best interest of the baby..
THE LABOUR :
The following morning after the check-up, I woke up for Fajr prayers, and realized that my waterbag has broken..It was about 6.45am..I woke hubby up and told him..
Then I packed up my hospital bag..and also packed up my elder's daughter bag (to send her to her grandma's).
I told hubby to get some rest as it's gonna be a long day :-)
Then he woke up at about 9.30a.m, saying he's worried that I would be in pain and couldn't sleep anymore. At that point of time, I had no pain yet, just discomfort from the water gushing out.
So we had roti canai for breakfast, and left house at about 11 a.m. We sent off my elder daughter and the maid to my MIL before going to the hospital.While on the way, I took sips of water which I soaked Bunga Kembang Fatimah with (it's suppose to help to accelerate labour).
We reached hospital at about 12 p.m and went straight to labour room. I felt my first contraction while we were in the car. At the labour room, the midwife checked and said that it was going to be a long way till delivery because cervix wasn't favourable at all..At about 1pm, my OBGYN came and did a V.E. She said I was already 2cm open..Alhamdulillah! However, she suggested that I was started on Pitocin to speed up the labour (with the reasons that I had been leaking liquor for some time and she did not want any infection to develop if the labour took "too long". She also was worried that a long labour might accentuate my hypertension). At that moment, I consented.
So she asked if i wanted epidural..I declined because I didn't like the idea of a needle poking nearby my spinal cord and also didn't want the side effects afterwards. I didn't take it for my first delivery, so I thought probably I might not need it this time as well..
At about 2p.m, I felt intense pain, and was already 3cm open. I requested for pethidine, and was given a shot. My BP shot up at that moment of time too so they gave me some anti-hypertensives and off the lights and told me to rest..
After that, I couldn't remember quite clearly anymore..All I knew was I keep waking up because of the intense pain..and at about 5pm, was told that I was 5cm open..and about 30 minutes later, I felt like pushing already..I told the nurse to check and to her surprise, I was already fully dilated and baby's head was ready to pop out..
So I started pushing, but to my despair, the nurse took a sanitary pad and blocked the opening, told me to stop pushing until the OBGYN comes. I was so angry at that point, I started shouting away. Luckily, the OBGYN arrived soon and only after 1 push, the baby was out! Alhamdulillah, I heard her cry and all the pain went away after that. To my delight, I was told that perineum was intact and no stitches were needed.
 |
| My 2nd Daughter (Nur Nabeeha) |
 |
| When two sisters meet for the first time :-) |
I was saddened that they did not allow me skin to skin time with my baby with the excuse that baby was small and had to be put to warmer. It really did hurt me but I was too weak to fight for it at that moment.
All I was thinking about was how glad I was to have delivered a healthy baby!
So overall, my active phase of labour this time was only about 5 hours, Alhamdulillah..compared to the 12 hours the previous time. I probably could give some credit to me making a habit to walk at least 15 minutes daily this time around :-) Hubby was there all the way beside me, giving me support and reminding me to be patient and salawat as much as I can..He was a gem at that moment, I cound't thank him enough..I held his hand all the way through the contraction pains..
Alhamdulillah for the fast and safe delivery :-)
As for my blood pressure, it went back to normotensive state about 2 weeks post-partum :-)
Even with the bad experiences during the labor this time around, I am thankful for a safe delivery and healthy baby, Alhamdulillah!
The past two birth experiences has encouraged me to look deeper into Gentle Birthing and hopefully I get a peaceful, calm gentle birth the next time around, InshaAllah!
Sunday, 13 April 2014
My 1st Pregnancy & Birth Story
Assalamualaikum.
This is indeed the first entry of this blog, Alhamdulillah.
Honestly, I was thinking of where and how to start and it clicked to me that probably I should start with my personal birth stories. That way, it would be a good platform of me introducing why I am taking up the AMANI Birth Childbirth Educator training and what I wish to convey to all mothers and mothers to be, InshaAllah.
Do take note however, that even though I delivered both my daughters vaginally, both deliveries were not all natural/gentle birthings. InshaAllah, I will discuss on various topics/issues with regards to my birthing experiences in following posts.
Overall, my first pregnancy was a healthy one except I had two episodes of bleeding during 6 weeks gestation and 8 weeks gestation. Both bleeding episodes lasted for a week with bright red to gradually brownish blood. It was diagnosed as threatened miscarriage but Alhamdulillah, the pregnancy survived!
I was adviced bed rest during the bleeding episodes and was also given some hormonal medication (Duphaston). I took the medications but didn't manage to get complete bed rest because I had to attend my classes and hospital bedside teachings, but at home, Hubby made sure I got ample bed rest (he took care of our meals and household chores). He also carried my to the bedroom (our bedroom was upstairs and I was adviced not to climb stairs). Luckily, I was still lightweight at that time! :-)
Honestly, I will want to look further into bed rest during bleeding in early pregnancy. I have heard so much of it, but have not came accross a study which really proves it's efficacy. Hopefully I will have time to look it up soon, InshaAllah..
Moving on to my labour story..
On a Friday night, 16/5/2008 (when my baby was 39 weeks 2 days gestation)..while I was watching television at around 8pm..felt my back aching and the kind of pain when my menses was going to come..
Hesitated to call hubby as he was in Tesco, doing some groceries shopping. Anyway, the pain was gradually intensifying but still torelable..and I decided to call him as I was alone and also quite scared :-)
He came back immediately after receiving my call and we went to my dear OBGYN, the loud but kind lady doctor.
Alhamdulillah..after a V.E, she said I was 1cm open, and my cervix was favourable. She gave us two options. First was to go back home, rest, let labour progress naturally and get admitted to hospital when contractions started or intensified (which could take a few hours to a few days according to her). Second option was to get admitted to hospital tonight, and augment the labour if it did not show any signs of progress by tomorrow morning.
Hubby left the decision to me, and I asked, " if I chose the second option, my baby would be delivered by tomorrow right?" My OBGYN said "Yes"..So I agreed for the second option. My OBGYN then asked me to have a good dinner and get myself admitted by tonight.
Let me explain on why I chose the second option, which is to augment the labour. Hubby and me were final year medical students at that moment. In our institution, there was no such thing as "maternity leave". And there was a certain limit of attendance of which we have to achieve to be able to sit for our exams. It so happens that it was a Friday night and also a start of 2 week term break. So I thought, the timing was right, because if I delivered the next day, I could at least have 2 weeks of break and fully spend time with my baby for 2 weeks to get some nesting in time and establish breastfeeding. At 38 weeks of pregnancy, hubby and me had saved up to hire a helper to help take care of the baby while we were attending classes. So I thought, two weeks was a short but at least some ample time for me to also get the helper familiarized with the baby before I start classes. Therefore, I chose the second option. Might not be the wisest choice, but God knows at that moment, it did really seem like the right choice..
Back to the labour story..
So my hubby asked what I wanted to eat, and I said `Lets go eat TOMYAM' . So we had dinner at a restaurant..and headed home to shower and bring along the `BUNGA KEMBANG FATIMA' which my mother in law brought from Mecca (a kind of flower which blooms when you soak it in water..Supposed to help facilitate labour).
-checked in at midnight
-7.00 a.m next morning, V.E showed still no improvemt in cervix dilatation..there were contractions but mild and very far apart..so we decided to augment using pitocin. I was also strapped up with the fetal monitoring machine, and it did feel very restrictive and uncomfortable. However, I did not mind at that moment because I was too nervous to walk about :-)
-7.30 a.m..I was on pitocin infusion..and contractions started becoming stronger..my gynae already warned she didn't want me on epidural or painkillers (saying that it would make me lazy to push later because I didn't feel pain)
-12 p.m..still tolerating the pain..only 3cm open..hubby got me lunch (rice, chicken and vege) and convinced me to eat, saying I need energy to push later..he fed me lunch and I actually finished the whole plate.
-1:00 p.m..waterbag broke..gush came the amniotic fluid..felt like a balloon popping in my tummy..
at that point I was begging for painkillers, so the midwife came to my aid and gave me a jab of pethidine at the gluteal region..
-Slept....hearing my hubby's voice reciting Yassin beside me..I literally though I was dead and asked him "Am I alive?" He just comforted me..and he reminded me to keep on salawat.
-4:00 p.m..V.E showed 6cm dilated..begged for another jab of painkiller..all was fuzzy during that time..was just sleeping and waking up time to time in pain..
-6.30pm...heard my loud gynae's voice waking me up..she said I was ready to push..
My hubby said that I was actually smiling when I heard that..Of course !..I was happy that it was end of the journey of labor..Alhamdulillah, my OBGYN told my hubby to support by back and thought me the sitting squatting position..She thought me how to wait until contraction started, take some deep breathes and when I am ready, to take a long deep breath and push as long as I can while holding my breath..Alhamdulillah, I was concious enough to co-operate and I was ready to strive till the end..
I felt my OBGYN do an episiotomy but did not feel any pain from it at that moment. I presume it was a compression episiotomy which she did during crowning..
Alhamdulillah, after 3 pushes,and at 6:48p.m..I heard my baby's cry and all the pain went away..My husband caught her himself and she came out smiling with eyes open according to him, MashaAllah!
A healthy 2.65kg baby girl!
The birthing staff did put my baby on my chest but I was too weak to even hold my baby..I think we managed to achieve some delayed cord clamping because Hubby was busy snapping photos of my little girl and the staff let him do it before proceeding to cut the cord, Alhamdulillah! You may see the photo with the vernix and fresh cord, Subhanallah!
Moments later, I felt some blood gushing and placenta came out naturally Alhamdulillah..The OBGYN stitched my episiotomy while my baby got cleaned up and weighed.
After the stitching and fussing over me was done, I was pushed in a wheel chair from the delivery room to the ward room. On the way, I asked to stop by the nursery so I could hold my baby for a while. MashaAllah, she was all alert and smiles despite the pethidine! I held her for just a few seconds, but I was so dizzy and afraid of dropping her, so I put her back in the cot.
At the ward room, my mother attempted to feed me dinner, but I vomited out everything (probably because of the analgesics). I lied down for a while and when my relatives were back home, I asked for my baby at night (about 9 pm) and we had a quite moment just staring at each other and I attempted to nurse her, Alhamdulillah..MashaAllah, I can never forget that quiet moment, just the two of us..
Hubby came in a little while later, and he joined the bonding moment, just the three of us.
We got some rest and Alhamdulillah, was discharged the next morning..
This is indeed the first entry of this blog, Alhamdulillah.
Honestly, I was thinking of where and how to start and it clicked to me that probably I should start with my personal birth stories. That way, it would be a good platform of me introducing why I am taking up the AMANI Birth Childbirth Educator training and what I wish to convey to all mothers and mothers to be, InshaAllah.
Do take note however, that even though I delivered both my daughters vaginally, both deliveries were not all natural/gentle birthings. InshaAllah, I will discuss on various topics/issues with regards to my birthing experiences in following posts.
Overall, my first pregnancy was a healthy one except I had two episodes of bleeding during 6 weeks gestation and 8 weeks gestation. Both bleeding episodes lasted for a week with bright red to gradually brownish blood. It was diagnosed as threatened miscarriage but Alhamdulillah, the pregnancy survived!
I was adviced bed rest during the bleeding episodes and was also given some hormonal medication (Duphaston). I took the medications but didn't manage to get complete bed rest because I had to attend my classes and hospital bedside teachings, but at home, Hubby made sure I got ample bed rest (he took care of our meals and household chores). He also carried my to the bedroom (our bedroom was upstairs and I was adviced not to climb stairs). Luckily, I was still lightweight at that time! :-)
Honestly, I will want to look further into bed rest during bleeding in early pregnancy. I have heard so much of it, but have not came accross a study which really proves it's efficacy. Hopefully I will have time to look it up soon, InshaAllah..
Moving on to my labour story..
On a Friday night, 16/5/2008 (when my baby was 39 weeks 2 days gestation)..while I was watching television at around 8pm..felt my back aching and the kind of pain when my menses was going to come..
Hesitated to call hubby as he was in Tesco, doing some groceries shopping. Anyway, the pain was gradually intensifying but still torelable..and I decided to call him as I was alone and also quite scared :-)
He came back immediately after receiving my call and we went to my dear OBGYN, the loud but kind lady doctor.
Alhamdulillah..after a V.E, she said I was 1cm open, and my cervix was favourable. She gave us two options. First was to go back home, rest, let labour progress naturally and get admitted to hospital when contractions started or intensified (which could take a few hours to a few days according to her). Second option was to get admitted to hospital tonight, and augment the labour if it did not show any signs of progress by tomorrow morning.
Hubby left the decision to me, and I asked, " if I chose the second option, my baby would be delivered by tomorrow right?" My OBGYN said "Yes"..So I agreed for the second option. My OBGYN then asked me to have a good dinner and get myself admitted by tonight.
Let me explain on why I chose the second option, which is to augment the labour. Hubby and me were final year medical students at that moment. In our institution, there was no such thing as "maternity leave". And there was a certain limit of attendance of which we have to achieve to be able to sit for our exams. It so happens that it was a Friday night and also a start of 2 week term break. So I thought, the timing was right, because if I delivered the next day, I could at least have 2 weeks of break and fully spend time with my baby for 2 weeks to get some nesting in time and establish breastfeeding. At 38 weeks of pregnancy, hubby and me had saved up to hire a helper to help take care of the baby while we were attending classes. So I thought, two weeks was a short but at least some ample time for me to also get the helper familiarized with the baby before I start classes. Therefore, I chose the second option. Might not be the wisest choice, but God knows at that moment, it did really seem like the right choice..
Back to the labour story..
So my hubby asked what I wanted to eat, and I said `Lets go eat TOMYAM' . So we had dinner at a restaurant..and headed home to shower and bring along the `BUNGA KEMBANG FATIMA' which my mother in law brought from Mecca (a kind of flower which blooms when you soak it in water..Supposed to help facilitate labour).
-checked in at midnight
-7.00 a.m next morning, V.E showed still no improvemt in cervix dilatation..there were contractions but mild and very far apart..so we decided to augment using pitocin. I was also strapped up with the fetal monitoring machine, and it did feel very restrictive and uncomfortable. However, I did not mind at that moment because I was too nervous to walk about :-)
 |
| A snapshot of our labor room. Alhamdulillah, I didnt' have to give birth lying on my back with legs hanging in the air. |
-7.30 a.m..I was on pitocin infusion..and contractions started becoming stronger..my gynae already warned she didn't want me on epidural or painkillers (saying that it would make me lazy to push later because I didn't feel pain)
-12 p.m..still tolerating the pain..only 3cm open..hubby got me lunch (rice, chicken and vege) and convinced me to eat, saying I need energy to push later..he fed me lunch and I actually finished the whole plate.
-1:00 p.m..waterbag broke..gush came the amniotic fluid..felt like a balloon popping in my tummy..
at that point I was begging for painkillers, so the midwife came to my aid and gave me a jab of pethidine at the gluteal region..
-Slept....hearing my hubby's voice reciting Yassin beside me..I literally though I was dead and asked him "Am I alive?" He just comforted me..and he reminded me to keep on salawat.
-4:00 p.m..V.E showed 6cm dilated..begged for another jab of painkiller..all was fuzzy during that time..was just sleeping and waking up time to time in pain..
-6.30pm...heard my loud gynae's voice waking me up..she said I was ready to push..
My hubby said that I was actually smiling when I heard that..Of course !..I was happy that it was end of the journey of labor..Alhamdulillah, my OBGYN told my hubby to support by back and thought me the sitting squatting position..She thought me how to wait until contraction started, take some deep breathes and when I am ready, to take a long deep breath and push as long as I can while holding my breath..Alhamdulillah, I was concious enough to co-operate and I was ready to strive till the end..
I felt my OBGYN do an episiotomy but did not feel any pain from it at that moment. I presume it was a compression episiotomy which she did during crowning..
Alhamdulillah, after 3 pushes,and at 6:48p.m..I heard my baby's cry and all the pain went away..My husband caught her himself and she came out smiling with eyes open according to him, MashaAllah!
A healthy 2.65kg baby girl!
The birthing staff did put my baby on my chest but I was too weak to even hold my baby..I think we managed to achieve some delayed cord clamping because Hubby was busy snapping photos of my little girl and the staff let him do it before proceeding to cut the cord, Alhamdulillah! You may see the photo with the vernix and fresh cord, Subhanallah!
Moments later, I felt some blood gushing and placenta came out naturally Alhamdulillah..The OBGYN stitched my episiotomy while my baby got cleaned up and weighed.
After the stitching and fussing over me was done, I was pushed in a wheel chair from the delivery room to the ward room. On the way, I asked to stop by the nursery so I could hold my baby for a while. MashaAllah, she was all alert and smiles despite the pethidine! I held her for just a few seconds, but I was so dizzy and afraid of dropping her, so I put her back in the cot.
At the ward room, my mother attempted to feed me dinner, but I vomited out everything (probably because of the analgesics). I lied down for a while and when my relatives were back home, I asked for my baby at night (about 9 pm) and we had a quite moment just staring at each other and I attempted to nurse her, Alhamdulillah..MashaAllah, I can never forget that quiet moment, just the two of us..
Hubby came in a little while later, and he joined the bonding moment, just the three of us.
We got some rest and Alhamdulillah, was discharged the next morning..
Sunday, 23 March 2014
Breast Compression
The purpose of breast compression is to continue the flow of milk to the baby once the baby no longer drinks (open-pause-close type of suck) on his own. Breast compression simulates a letdown reflex and often stimulates a natural letdown reflex to occur.
The technique may be useful for:
1. Poor weight gain in the baby
2. Colic in the breastfed baby
3. Frequent feedings and/or long feedings
4. Sore nipples in the mother
5. Recurrent blocked ducts and/or mastitis
6. Encouraging the baby who falls asleep quickly to continue drinking
Breast compression is not necessary if everything is going well. When all is going well, the mother should allow the baby to "finish" feeding on the first side and, if the baby wants more, should offer the other side. How do you know the baby is finished? When he no longer drinks at the breast (open-pause-close type of suck).It may be useful to know that:
1. A baby who is well latched on gets milk more easily than one who is not. A baby who is poorly latched on can get milk only when the flow of milk is rapid. Thus, many mothers and babies do well with breastfeeding in spite of a poor latch, because most mothers produce an abundance of milk.
2. In the first 3-6 weeks of life, babies fall asleep at the breast when the flow of milk is slow, not necessarily when they have had enough to eat. After this age, they may start to pull away at the breast when the flow of milk slows down.
3. Unfortunately many babies are latching on poorly. If the mother's supply is abundant the baby often does well as far as weight gain is concerned, but the mother may pay a price-sore nipples, a "colicky" baby, a baby who is constantly on the breast (but feeding only a small part of the time).
Breast compression continues the flow of milk once the baby starts falling asleep at the breast and results in the baby:
1. Getting more milk.
2. Getting more milk that is high in fat.
Breast Compression-How to do it
1. Hold the baby with one arm.
2. Hold the breast with the other, thumb on one side of the breast, your other fingers on the other, fairly far back from the nipple.
3. Watch for the baby's drinking, though there is no need to be obsessive about catching every suck. The baby gets substantial amounts of milk when he is drinking with an open-pause-close type of suck. (open-pause-close is one suck, the pause is not a pause between sucks).
4. When the baby is nibbling or no longer drinking with the open-pause-close type of suck, compress the breast. Not so hard that it hurts and try not to change the shape of the areola (the part of the breast near the baby's mouth). With the compression, the baby should start drinking again with the open-pause-close type of suck.
5. Keep the pressure up until the baby no longer drinks even with the compression, then release the pressure. Often the baby will stop sucking altogether when the pressure is released, but will start again shortly as milk starts to flow again. If the baby does not stop sucking with the release of pressure, wait a short time before compressing again.
6. The reason to release the pressure is to allow your hand to rest, and to allow milk to start flowing to the baby again. The baby, if he stops sucking when you release the pressure, will start again when he starts to taste milk.
7. When the baby starts sucking again, he may drink (open-pause-close). If not compress again as above.
8. Continue on the first side until the baby does not drink even with the compression. You should allow the baby to stay on the side for a short time longer, as you may occasionally get another letdown reflex and the baby will start drinking again, on his own. If the baby no longer drinks, however, allow him to come off or take him off the breast.
9. If the baby wants more, offer the other side and repeat the process.
10. You may wish, unless you have sore nipples, to switch sides back and forth in this way several times.
11. Work on improving the baby's latch.
The above works best, in our experience in the clinic, but if you find a way which works better at keeping the baby sucking with an open-pause-close type of suck, use whatever works best for you and your baby. As long as it does not hurt your breast to compress, and as long as the baby is "drinking" (open-pause-close type of suck), breast compression is working.You will not always need to do this. As breastfeeding improves, you will able to let things happen naturally
Saturday, 1 February 2014
Getting a Good Start in Breastfeeding
11. Starting Out Right
(a) Prepare yourself mentally and physically, starting as early as during pregnancy.
Gather as much information about pregnancy, childbirth and breastfeeding as you can through trusted resources. When you are well-equipped with knowledge, you will understand what you are going through, will know what to expect and will be able to plan how to deal with it. With 101 myths on motherhood and breastfeeding that community tend to spread around, knowledge serves as a shield to protect you against being deviated against breastfeeding.
Start practising a healthy lifestyle like good eating, sleeping and exercise habits, to keep yourself healthy physically so that when your bundle of joy arrives, you will able provide him/her the best of care. Having said that, each mother is different so I am not able to touch on what I mean when I mentioned good eating/exercise habits because this varies from individual to individual.
(b) Equip yourself with appropriate breastfeeding tools
Yes mothers, I know how it feels when you go shopping for your expected newborn. Especially if it’s a girl! You would feel like grabbing all the gorgeous clothes from the racks. But trust me dear mothers, investing in proper equipments for breastfeeding is way much more important. I learnt this by mistake from my first pregnancy. I spent on clothes until some of the clothes my baby didn’t even get the chance to wear because she outgrew it! I didn’t even think of buying a breastpump, let alone other equipments at that moment. So, the outcome was, my breastfeeding attempt tallied to my breastfeeding effort, in which of course, I failed. Shame on me. We all learn from mistakes, I suppose. Anyway, I was more cautious during my second pregnancy, and prepared all the basic stuff needed for breastfeeding to work.
It may be "expensive" to start out, but it is a once for all investment. If you do the math and calculate the price for formula milk for two years versus your one time investment for breastfeeding tools (which can last for two years if you care for it meticulously), breastfeeding is still cheaper. Another plus point in saving money is that breastfed babies have less hospital visits compared to formula fed babies.
(c) Choosing the right hospital and informing hospital staffs regarding your wish to breastfeed.
Baby friendly hospitals are generally much more co-operative than those which are not. If you plan to deliver in a non-baby friendly hospital, inform the staffs beforehand regarding your wish to breastfeed. Make a tag stating `Fully Breastfeeding’ and as the nurse to stick in on your babies cot in the hospital nursery.
Having said all the above, I made mistakes with my two previous deliveries. I gave birth in a non-baby friendly hospital, thinking that all hospitals would support breastfeeding. I literally had to beg the nurses to bring my baby to me for feeding. I was given weird stares by nurses when my baby cried after two hours of latching on the breast. I was given comments like `Oh, you are not producing enough for you baby, that’s why she’s crying after nursing on the breast. We will top up 2 ounces of formula feed for her’. Best part, my baby was just a day old at that moment. And poor me who was so determined to breastfeed became so devastated and confused that I didn’t have the will to fight for my right at that moment. I sincerely hope mothers out there learn from my mistakes and do not have to go through what I went through.
2. Hard Work
2. Hard Work
Once you get home, continue nursing your baby directly as frequently as you can. Try to get the baby to latch on correctly to your breasts. This might take some time and patience, so do not give up if you failed the first few times. Try to start pumping as early as 1 week postpartum, whenever you have a break from the baby. If the baby wakes up while you are pumping, nurse him/her first then continue pumping. I know how tiring it can be to care for newborns, and I agree that mothers should take naps whenever baby is asleep. In that case, I may suggest nursing your child on one breast and pumping on the other side. This method can help prevent a mother becoming lopsided, help her build up her milk supply and help her prepare some milk stock (useful for working mothers when they get back to work).
-Have a method of monitoring your milk supply. Chart how much you pump a day and assess the baby’s intake in the form of weight gain, stool and urination.
-Breasts might not need cleaning after feeding, but if you are using the breastpump, all parts have to be cleansed and sterilized appropriately.
-Milk storage can also be a tideous process provided you have a system. Only store milk in bottles or bags meant for milk storage. Label the bottles/bags with date and time, so that first one in would be first one out.
3. Consistency
For working mothers, going back to work should not be a barrier for you to breastfeed. Discuss with your superiors regarding your need to pump at work. Plan your time and proper milk storage accordingly especially if your work involves a lot of travelling.
4. Adequate support from surroundings
-This is one of the most difficult factor pertaining to making breastfeeding work. There are abundance of negativism, criticism and inappropriate so-called advices rather than optimism, encouragement and co-operation. Sad to say, sometimes our own closest family members are against breastfeeding.
-Do attend Breastfeeding Classes with your companion (eg husband, mother) or the person who is going to help take care of you during confinement and so forth. It might help them understand the support you need with regards to breastfeeding.
-Should you encounter any lactation problems, search for a lactation consultant to help you overcome those problems and never resort to formula milk right away.
-My advice to mothers out there, do not let others cause your high spirited will to breastfeed crumble or shatter your emotions into pieces. Stay strong and remember that you are doing this for your baby and you so it doesn’t matter what others perceive.
Subscribe to:
Posts (Atom)