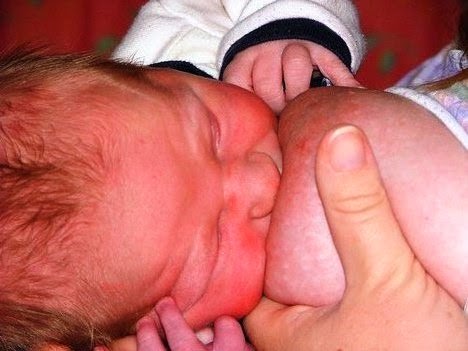
The purpose of breast compression is to continue the flow of milk to the baby once the baby no longer drinks (open-pause-close type of suck) on his own. Breast compression simulates a letdown reflex and often stimulates a natural letdown reflex to occur.
The technique may be useful for:
1. Poor weight gain in the baby
2. Colic in the breastfed baby
3. Frequent feedings and/or long feedings
4. Sore nipples in the mother
5. Recurrent blocked ducts and/or mastitis
6. Encouraging the baby who falls asleep quickly to continue drinking
Breast compression is not necessary if everything is going well. When all is going well, the mother should allow the baby to "finish" feeding on the first side and, if the baby wants more, should offer the other side. How do you know the baby is finished? When he no longer drinks at the breast (open-pause-close type of suck).It may be useful to know that:
1. A baby who is well latched on gets milk more easily than one who is not. A baby who is poorly latched on can get milk only when the flow of milk is rapid. Thus, many mothers and babies do well with breastfeeding in spite of a poor latch, because most mothers produce an abundance of milk.
2. In the first 3-6 weeks of life, babies fall asleep at the breast when the flow of milk is slow, not necessarily when they have had enough to eat. After this age, they may start to pull away at the breast when the flow of milk slows down.
3. Unfortunately many babies are latching on poorly. If the mother's supply is abundant the baby often does well as far as weight gain is concerned, but the mother may pay a price-sore nipples, a "colicky" baby, a baby who is constantly on the breast (but feeding only a small part of the time).
Breast compression continues the flow of milk once the baby starts falling asleep at the breast and results in the baby:
1. Getting more milk.
2. Getting more milk that is high in fat.
Breast Compression-How to do it
1. Hold the baby with one arm.
2. Hold the breast with the other, thumb on one side of the breast, your other fingers on the other, fairly far back from the nipple.
3. Watch for the baby's drinking, though there is no need to be obsessive about catching every suck. The baby gets substantial amounts of milk when he is drinking with an open-pause-close type of suck. (open-pause-close is one suck, the pause is not a pause between sucks).
4. When the baby is nibbling or no longer drinking with the open-pause-close type of suck, compress the breast. Not so hard that it hurts and try not to change the shape of the areola (the part of the breast near the baby's mouth). With the compression, the baby should start drinking again with the open-pause-close type of suck.
5. Keep the pressure up until the baby no longer drinks even with the compression, then release the pressure. Often the baby will stop sucking altogether when the pressure is released, but will start again shortly as milk starts to flow again. If the baby does not stop sucking with the release of pressure, wait a short time before compressing again.
6. The reason to release the pressure is to allow your hand to rest, and to allow milk to start flowing to the baby again. The baby, if he stops sucking when you release the pressure, will start again when he starts to taste milk.
7. When the baby starts sucking again, he may drink (open-pause-close). If not compress again as above.
8. Continue on the first side until the baby does not drink even with the compression. You should allow the baby to stay on the side for a short time longer, as you may occasionally get another letdown reflex and the baby will start drinking again, on his own. If the baby no longer drinks, however, allow him to come off or take him off the breast.
9. If the baby wants more, offer the other side and repeat the process.
10. You may wish, unless you have sore nipples, to switch sides back and forth in this way several times.
11. Work on improving the baby's latch.
The above works best, in our experience in the clinic, but if you find a way which works better at keeping the baby sucking with an open-pause-close type of suck, use whatever works best for you and your baby. As long as it does not hurt your breast to compress, and as long as the baby is "drinking" (open-pause-close type of suck), breast compression is working.You will not always need to do this. As breastfeeding improves, you will able to let things happen naturally